How to Evaluate Clinical Outcomes Articles for Improved Patient Care?
In the realm of healthcare, evaluating clinical outcomes articles is crucial for enhancing patient care. Dr. John Smith, a renowned expert in clinical research, stated, "Quality outcomes drive better healthcare decisions." This underscores the importance of scrutinizing these articles to improve treatment and patient satisfaction.
Clinical outcomes articles provide insights that can guide healthcare professionals. These insights help identify effective treatments and potential risks. However, not all articles are created equal. It's essential to discern the rigor behind the methodologies and the validity of conclusions drawn. Sometimes, findings may be published without adequate peer review, leading to questionable reliability.
Attention to detail in assessing these articles can lead to significant improvements in practice. Recognizing biases, limitations, and the context of the research will refine decision-making. As healthcare evolves, the need for reliable clinical outcomes articles becomes ever more essential. By emphasizing critical evaluation, we can ensure better clinical practices and, ultimately, improved patient care.
Understanding the Importance of Clinical Outcomes in Patient Care
Evaluating clinical outcomes is crucial for enhancing patient care. These outcomes provide insights into the effectiveness of treatments. Understanding these metrics is vital for healthcare professionals. They guide decisions and improve overall patient experiences. By focusing on clinical outcomes, healthcare providers can tailor their approaches, ensuring each patient receives the best possible care.
Tips for evaluating clinical outcomes include looking for data from reputable sources. Peer-reviewed journals often provide reliable information. Investigate the methodologies used in studies. Good research should have clear, transparent methods. Always consider the sample size in studies. Larger sample sizes generally offer more reliable results. Don't overlook the importance of follow-up data; it shows long-term effects on patient health.
Being aware of biases in clinical outcomes is necessary. Sometimes, results may not reflect the true picture. Diverse populations often yield different outcomes. This variation highlights the need for tailored healthcare solutions. A critical eye can help spot flaws in studies, leading to better patient care strategies. Engaging continuously with the data fosters improvements in clinical practices.
Key Metrics for Evaluating Clinical Outcomes Effectively
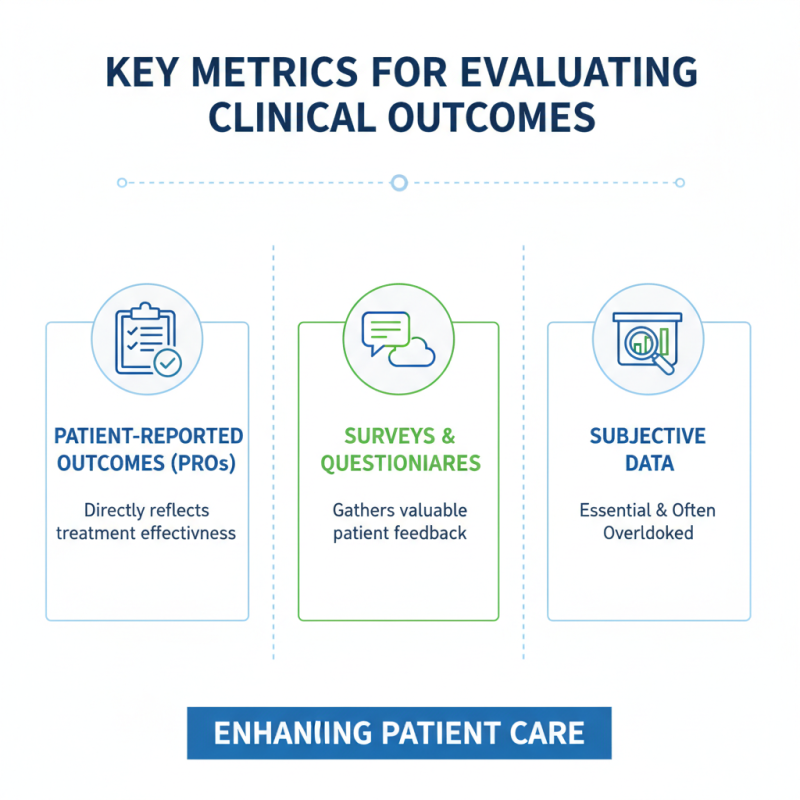
Evaluating clinical outcomes is crucial for enhancing patient care. Key metrics play a vital role in this assessment. A focus on patient-reported outcomes (PROs) can directly reflect treatment effectiveness. Surveys and questionnaires can help gather valuable feedback from patients. This subjective data is essential and often overlooked.
Another important metric is clinical effectiveness. This involves measuring outcomes such as mortality rates, hospital readmission rates, and complication statistics. These hard data points provide a clear picture of treatment success. However, drawing conclusions from these metrics requires caution. Variability in patient demographics can skew results, leading to potentially misleading interpretations.
Furthermore, consider the impact of patient engagement on outcomes. Engaged patients often adhere better to treatment plans. Analyzing the levels of involvement can provide insight into care quality. Assessing these areas isn’t always straightforward. There may be gaps in data that complicate evaluations. Continuous reflection and adjustment of evaluation strategies are essential for achieving the best outcomes.
Methods for Analyzing Clinical Outcomes Data
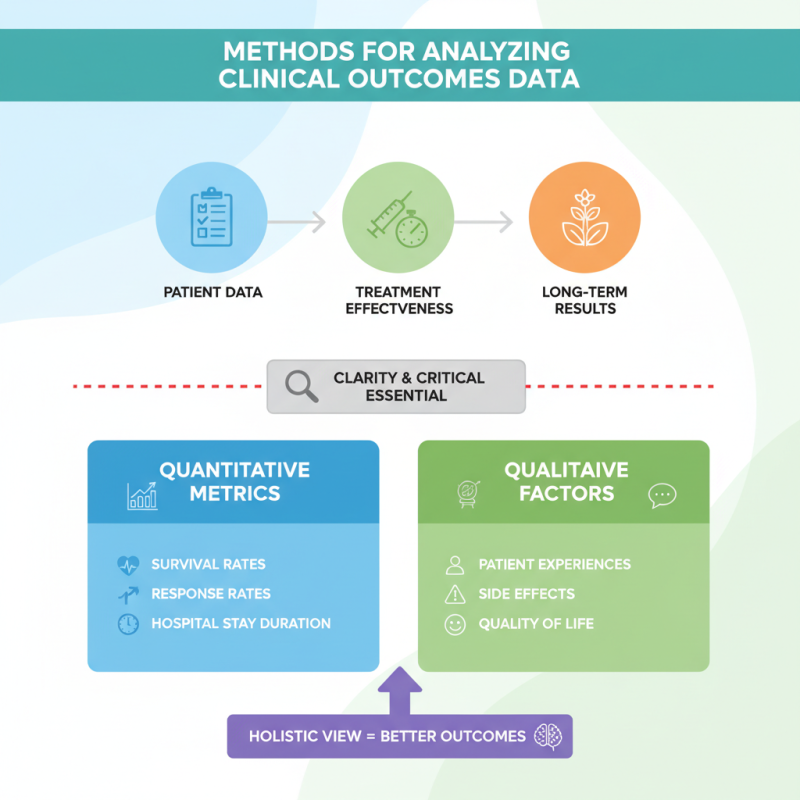
When analyzing clinical outcomes data, clarity is essential. Researchers often gather patient data, treatment effectiveness, and long-term results, but they must stay critical. The methods used for analysis can significantly impact outcomes. Relying solely on quantitative metrics may overlook qualitative factors. Patient experiences, side effects, and quality of life can be as crucial as survival rates.
Statistical analyses such as regression models are common. These help identify trends and correlations. However, these techniques can mislead if not interpreted cautiously. A correlation does not always imply causation. Peer-reviewed literature emphasizes the need for comprehensive data assessments. Integrating clinical expertise with statistical findings is vital.
Additionally, outcomes should be reviewed frequently. A study may show results after one year but change in longer follow-ups. Continuous monitoring and adjustment based on new evidence are necessary. Engaging with diverse stakeholders, including patients, enhances understanding. This collaboration promotes a well-rounded perspective on clinical outcomes. Exploring these elements can facilitate improved patient care.
Integrating Clinical Outcomes into Patient Care Strategies
Integrating clinical outcomes into patient care strategies significantly enhances treatment effectiveness. Care providers must focus on data-driven approaches that reflect real-world patient experiences. Successful integration can lead to better health outcomes and improved patient satisfaction. It’s essential to evaluate clinical outcomes to align them with individual patient needs.
To effectively incorporate clinical outcomes, consider these tips: Collaborate with multidisciplinary teams. Diverse professional insights can lead to better assessment and interpretation of data. Regularly review clinic protocols based on outcome evaluations. This ensures continuous improvement and relevance in treatment methods.
Patient feedback is invaluable. Actively seek it to understand the practical impact of your strategies. Personalizing care based on outcomes can bridge gaps in healthcare delivery. Reflect on the shortcomings in your approach. Recognize that not all interventions will yield expected results. This humility can foster growth and enhance your practice.
How to Evaluate Clinical Outcomes Articles for Improved Patient Care?
| Dimension | Description | Example Metrics |
|---|---|---|
| Patient Satisfaction | Measures the degree to which patients are happy with their healthcare experience. | Patient Satisfaction Surveys, Net Promoter Score (NPS) |
| Clinical Effectiveness | Evaluates how well a certain treatment or intervention works in clinical practice. | Improvement in Symptoms, Recovery Rates |
| Quality of Life | Assesses the overall well-being and functional status of patients. | Quality of Life Assessments, Functional Status Scales |
| Cost-effectiveness | Examines the economic impact of healthcare interventions. | Cost per Quality Adjusted Life Year (QALY) |
| Patient Safety | Measures the extent of harm or risk of harm to patients during healthcare delivery. | Incidence of Adverse Events, Medication Errors |
Best Practices for Continuous Improvement in Patient Outcomes
Evaluating clinical outcomes is crucial for enhancing patient care. Continuous improvement in patient outcomes requires actionable data. According to a recent report from the Institute of Medicine, nearly 30% of patients do not receive evidence-based care. This gap highlights the importance of translating clinical evidence into practice.
Healthcare professionals should utilize systematic reviews and meta-analyses when assessing new interventions. These resources help identify effective treatments and potential pitfalls. A study by the National Institutes of Health shows that adopting best practices can result in a 20% increase in patient satisfaction scores. Clear communication and education are essential. Engaging patients in their care can lead to better adherence and outcomes.
However, not all interventions yield the desired results. The challenge often lies in implementation, which can vary across settings. The Agency for Healthcare Research and Quality stresses the importance of tailoring strategies to specific contexts. Regular evaluation and adjustment based on patient feedback aid in refining approaches. Despite best efforts, some initiatives may not resonate, underscoring the need for ongoing learning and adaptation in the pursuit of improved patient care.
Related Posts
-
China Best Consensus Knee System Innovations and Benefits Explained?
-

2026 Top Innovations in Joint Replacement Featuring TaperSet Hip System?
-

Why Are FDA Approved Orthopedic Implants Essential for Successful Surgery?
-

Best Partial Knee Replacement Care Options Worldwide?
-
How to Choose the Best Hip Replacement Systems for Your Needs?
-

Top Orthopedic Implant Innovations Transforming Healthcare Today?
Why Shalby MedTech
We are committed to deliver solutions and transforming the way joint replacement procedures are performed.


 Looking for the
Looking for the  Register as
Register as